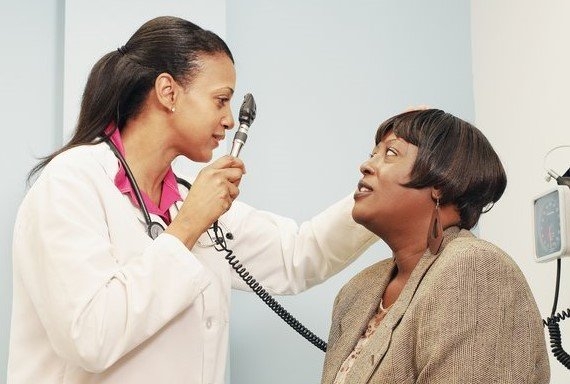
Sponsored by New York for Seniors | Home Care Seniors often experience different health challenges, including physical injuries as a result...
Mayor de Blasio told New Yorkers that they weren’t alone in yearning for a return to normal, but he said there’s still work to be done...
Continue reading
Amid the ongoing COVID-19 pandemic, five new testing facilities are opening, primarily in neighborhoods where the need is greatest. A...
Continue reading
Before the COVID-19 outbreak, Annette Adams-Brown’s 87-year-old mother was an avid follower of TV news. Now Adams-Brown has to...
Continue reading
NYC Department for the Aging (DFTA) is making it possible for seniors to have meals delivered to their homes. Direct delivery includes a...
Continue reading
By Beth Witrogen For 30 years, Robyn Yale has been on a mission to raise awareness that people with early-stage Alzheimer’s disease...
Continue reading
Today it was announced that CenterLight Healthcare has come on board as an event sponsor for the New York for Seniors Health & Wellness...
Continue reading
(HealthDay News) — If you had a heart attack and could get rehab therapy at home, would you be more likely to get the follow-up care...
Continue reading
JIG Media, the hyper-local digital marketing agency, located in DUMBO, Brooklyn, will be expanding its healthy living initiative in New...
Continue reading
Seniors Can Qualify for Medicaid & Receive Home Care Even if Their Income Exceeds the NY State Limit
The most common challenge for New York’s seniors looking to get home care, is qualifying for Medicaid, which will pay for the needed...
Continue reading
The standoff between the New York State Nurses Association and New York City’s three largest health systems, Mount Sinai, Montefiore...
Continue reading
YOU MUST REGISTER (RSVP) FOR THESE SESSIONS TO GET IN! New York for Seniors is hosting another Information Session for healthcare sales...
Continue reading
New York for Seniors is pleased to announce that Visiting Nurse Service of New York (VNSNY), will be on hand at the New York for Seniors...
Continue reading
Today it was announced that Bright Health has become a partner of the New York for Seniors Health & Wellness Resource Series. The...
Continue reading
Courtesy HHS.gov Generally, Medicare is available for people age 65 or older, younger people with disabilities and people with End Stage...
Continue reading
Leading up to the open-enrollment periods for Medicare and New York State of Health, the State’s official online marketplace, NYC Health...
Continue reading
What is Medicare? Medicare is the federal health insurance program for people who are 65 or older, certain younger people with...
Continue reading
Today, JIG Media and Mastermind Connect announced that Hope Home Care has joined the 2018 Healthy NYC Expo on Governors Island along with...
Continue reading
The Oxford Nursing Home, located in Ft Greene, Brooklyn, is looking to move to East New York. The new nursing home will change its name...
Continue reading
Tradition Home Care, a Brooklyn-based home care agency, has launched their new digital platform, which will make it easier for them to...
Continue reading
New York City Economic Development Corporation (NYCEDC) President and CEO James Patchett, City Council Speaker Melissa Mark-Viverito and...
Continue reading
Beacon Eldercare recently opened a new office in the heart of the bustling pedestrian shopping hub in Maspeth, Queens. The new office is...
Continue reading
Many seniors and caregivers might know JASA as an organization that operates senior centers, but they offer so much more, including Home...
Continue reading
New York’s Consumer-Directed Personal Assistance Program (CDPAP) has enrolled, in its nearly three decades of operation, around 10,000...
Continue reading
Managed Long Term Care (MLTC) is a system that streamlines the delivery of long term services to people who are chronically ill or disabled...
Continue reading
Health Care is extremely important for New York’s seniors right now, which makes it even more important to understand the...
Continue reading
What Is FIDA? FIDA stands for Fully Integrated Duals Advantages. It is a program that combines Medicare and Medicaid services together with...
Continue reading
Managed Long Term Care, or MLTC, is a plan that arranges long term services for homebound chronically ill or disabled people, and is...
Continue reading
Managed Care is a term that is used to describe a health insurance plan or health care system that coordinates the provision, quality and...
Continue reading
Managed Long Term Care (MLTC) is a system that streamlines the delivery of long term services to people who are chronically ill or disabled...